This chapter on Acne has been specifically prepared for candidates preparing for the Pharmacy Examining Board of Canada (PEBC) examinations. It provides essential information relevant for both the Evaluating Examination (EE) and the MCQ components. The content focuses on acne’s pathophysiology, clinical presentation, and treatment options, designed to help pharmacy students understand key concepts needed to manage acne effectively in clinical practice.
Introduction
Acne vulgaris is one of the most prevalent skin disorders worldwide, primarily affecting adolescents but also extending into adulthood for many individuals. It presents with a variety of skin lesions, including comedones (blackheads and whiteheads), papules, pustules, nodules, and cysts. Acne can lead to physical scarring and significant psychological distress, impacting self-esteem and quality of life even in mild cases.
Pathophysiology
Acne is a multifactorial inflammatory disease centered around the pilosebaceous units of the skin, which consist of hair follicles and their accompanying sebaceous glands. Four key factors contribute to the development of acne:
Follicular Hyperkeratinization: An abnormal shedding of skin cells within the hair follicle leads to clogging of the pores.
Increased Sebum Production: Hormonal changes stimulate the sebaceous glands to produce excessive sebum (oil), creating an environment conducive to acne formation.
Colonization by Cutibacterium acnes: Formerly known as Propionibacterium acnes, this bacterium thrives in the clogged follicles, exacerbating inflammation.
Inflammatory Responses: The body's immune reaction to bacterial proliferation and sebum leads to inflammation, resulting in the various types of acne lesions.
Other contributing factors may include hormonal imbalances, dietary influences (such as high glycemic load diets and dairy intake), genetic predisposition, and disruptions of the skin barrier.
Clinical Presentation
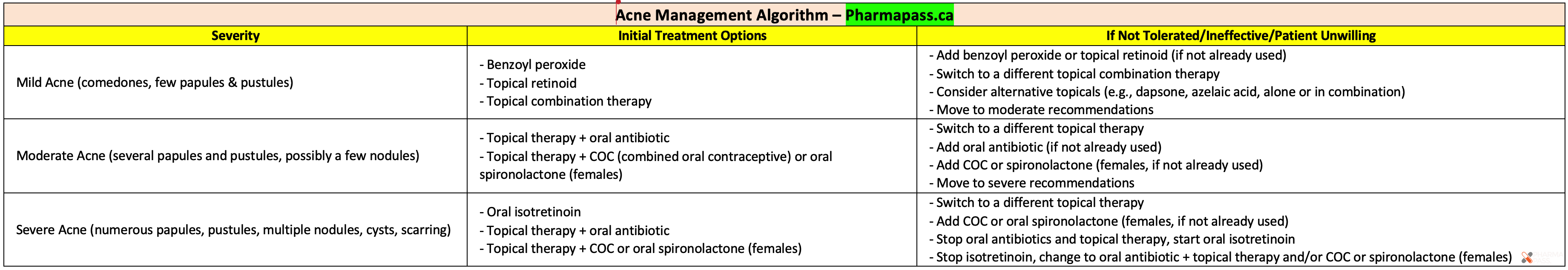
Acne lesions are typically classified based on their severity and the types of lesions present:
Mild Acne: Characterized by the presence of comedones with occasional small papules and pustules.
Moderate Acne: Includes numerous papules and pustules along with a few nodules.
Severe Acne: Features extensive papules, pustules, multiple nodules or cysts, and often results in scarring.
Common areas affected by acne include the face, chest, back, and shoulders, correlating with regions of higher sebaceous gland density.
Goals of Treatment
Effective acne management aims to:
Eliminate Existing Lesions: Reduce the number and severity of current acne spots.
Prevent New Lesion Formation: Inhibit the processes that lead to new acne development.
Minimize Scarring: Prevent permanent skin damage through early and appropriate treatment.
Reduce Hyperpigmentation: Address discoloration that may occur after lesions heal.
Improve Psychological Well-being: Alleviate the emotional and social impacts associated with acne.
Management Strategies
Non-Pharmacological Approaches
Gentle Skin Care: Cleanse the skin twice daily with a mild, non-abrasive cleanser to remove excess oil and impurities without causing irritation.
Avoid Manipulating Lesions: Picking or squeezing acne spots can worsen inflammation and increase the risk of scarring and infection.
Dietary Considerations: While the relationship between diet and acne is not fully established, some evidence suggests that reducing high glycemic foods and dairy intake may benefit some individuals.
Sun Protection: Use non-comedogenic sunscreen to protect the skin, as some acne treatments can increase sensitivity to sunlight.
Stress Management: Since stress can exacerbate acne, incorporating stress-reduction techniques like exercise, meditation, or adequate sleep may be helpful.
Pharmacological Treatments
Treatment choices depend on the severity of acne and individual patient factors. Often, a combination of therapies yields the best results.
Topical Therapies
Benzoyl Peroxide
Mechanism: Exhibits antibacterial properties by releasing free oxygen radicals that destroy bacteria. It also has mild comedolytic effects.
Usage: Available over-the-counter in concentrations ranging from 2.5% to 10%. Applied once or twice daily to affected areas.
Considerations: Can cause skin dryness and irritation; starting with lower concentrations may improve tolerance. May bleach fabrics and hair.
Topical Retinoids
Types: Tretinoin, Adapalene, Tazarotene, and Trifarotene.
Mechanism: Normalize keratinocyte shedding, preventing follicular plugging. Also possess anti-inflammatory properties.
Usage: Typically applied once daily at night due to photosensitivity risk.
Considerations: May cause irritation and dryness initially; using a moisturizer and gradual introduction can mitigate side effects.
Topical Antibiotics
Agents: Clindamycin and Erythromycin.
Mechanism: Reduce C. acnes colonization and inflammation.
Usage: Applied once or twice daily, often in combination with benzoyl peroxide to prevent antibiotic resistance.
Considerations: Should not be used as monotherapy due to resistance risk.
Azelaic Acid
Mechanism: Inhibits protein synthesis in C. acnes and normalizes keratinization.
Usage: Applied twice daily.
Considerations: Generally well-tolerated; may improve post-inflammatory hyperpigmentation.
Salicylic Acid
Mechanism: A beta-hydroxy acid that promotes exfoliation of the skin and unclogs pores.
Usage: Found in over-the-counter products in concentrations of 0.5% to 2%.
Considerations: Less potent than retinoids but may be better tolerated by sensitive skin.
Systemic Therapies
Oral Antibiotics
Agents: Doxycycline, Minocycline, Tetracycline, and Erythromycin.
Mechanism: Reduce bacterial colonization and inflammation.
Usage: Indicated for moderate to severe acne; typically used for limited durations (3-6 months).
Considerations: Side effects may include gastrointestinal upset and photosensitivity. Not recommended for long-term use due to resistance concerns.
Hormonal Therapies (for Females)
Combined Oral Contraceptives
Mechanism: Regulate hormonal fluctuations that contribute to sebum production.
Usage: Various formulations available; some contain anti-androgenic progestins.
Considerations: May have side effects like weight changes, mood alterations, and increased risk of thromboembolism.
Spironolactone
Mechanism: An anti-androgen that reduces sebum production.
Usage: Doses range from 50 to 200 mg daily.
Considerations: Monitor for hyperkalemia; not recommended during pregnancy.
Isotretinoin
Mechanism: A vitamin A derivative that dramatically reduces sebum production, normalizes keratinization, and has anti-inflammatory effects.
Usage: Reserved for severe nodulocystic acne or cases unresponsive to other treatments. Treatment courses typically last 16-20 weeks.
Considerations: Highly teratogenic—strict pregnancy prevention measures are necessary. Common side effects include dry skin, lips, and eyes; less common but serious effects can include liver enzyme elevations and mood changes.
Monitoring and Follow-up
Efficacy Assessment: Treatment effectiveness is usually evaluated after 6-8 weeks due to the skin's renewal cycle.
Side Effect Management: Address any adverse effects promptly to improve adherence.
Long-term Maintenance: Once acne is controlled, maintenance therapy (often with topical agents) may prevent relapse.
Special Considerations
Pregnancy and Acne
Safe Treatments: Topical azelaic acid and benzoyl peroxide are generally considered safe.
Avoided Treatments: Topical and oral retinoids, tetracycline antibiotics, and hormonal therapies should be avoided due to potential risks to the fetus.
Psychosocial Impact
Acne can significantly affect mental health, leading to anxiety, depression, and social withdrawal.
Supportive Measures: Counseling or support groups may benefit those experiencing psychological distress.
Conclusion
Acne is a complex condition with both physical and psychological ramifications. Understanding its pathophysiology is essential for effective management. Early intervention and a tailored treatment approach can significantly improve outcomes, reduce the risk of scarring, and enhance the quality of life for those affected. Ongoing research continues to shed light on new therapeutic options and strategies to combat this common skin disorder.